Antimicrobial resistance is a global health and development challenge that demands urgent and coordinated action
-

4.7 million deaths were associated with AMR in 2021.
Murray et al, The Lancet, 2024 (Ref. 1)
Photo by Paolo Nicolello on Unsplash
-

AMR costs EU/EEA countries €32.6 million every day.
Deducted from OECD, 2023 (Ref. 2)
Photo by Ibrahim Boran on Unsplash
-

Since 2017, 13 new antibiotics were authorized, but only 2 are from a new chemical class and considered innovative.
WHO, 2024 (Ref. 3)
Photo by ameenfahmy on Unsplash
Antimicrobial resistance (AMR) occurs when bacteria and other microbes learn to avoid the drugs that are meant to kill them - like antibiotics. This makes it much harder, and sometimes even impossible, to treat infections. These drug-resistant microbes, often called 'superbugs,' contributed to 4.7 million deaths in 2021.
Without urgent action, they could kill up to 8.2 million people each year by 2050 (1). AMR also presents a significant economic threat, with the potential to reduce global GDP by nearly 4% by 2050 (4). In Europe alone, the economic impact of AMR is projected to reach €11.7 billion annually in healthcare costs and lost productivity by 2050 (2).
The emergence of superbugs is due to decades of overuse and misuse of antibiotics, which has allowed bacteria to gradually develop resistance and turned a silent pandemic of antibiotic resistance into a global health crisis. Antibiotics are the backbone of modern medicine – they are used in everything from treating infections to safe surgeries and cancer treatment. If we lose them, we lose one of our most powerful tools to protect our health. AMR is recognized by WHO (2015) and EU (2017) as a top-level global health threat, requiring immediate and coordinated action (5,6). Because drug development spans many years, addressing antibiotic resistance requires decisive action starting now.
smartbax takes this action by developing a new generation of small-molecule antibiotics that outsmart bacteria and protect global health.
We focus exclusively on bacterial targets that are not addressed by existing antibiotics and specialize in the dysregulation of hydrolases which are critical for cellular integrity. Thus, our unique modes of action kill bacteria as they interfere in the production of essential cell wall components or induce an uncontrolled self-digest. smartbax has its academic roots in work from Prof. Stephan Sieber at the Technical University of Munich, where the discovery of a novel activator of the signal peptidase SpsB showed remarkable antibiotic potential (7). Starting from there, smartbax established a multi-modal development platform, with currently three independent projects in the pipeline, ranging from hit-to-lead to lead optimization.
References
1) Naghavi et al. (2024). Global burden of bacterial antimicrobial resistance 1990–2021: a systematic analysis with forecasts to 2050. The Lancet 404 (10459): 1199–1226.
2) OECD (2023). Fighting Antimicrobial Resistance in EU and EEA countries Embracing a One Health Approach.
3) WHO (2023) Antibacterial agents in clinical and preclinical development: an overview and analysis.
4) Rupasinghe et al. (2024). Stopping the Grand Pandemic: A Framework for Action - Addressing Antimicrobial Resistance through World Bank Operations. World Bank. https://doi.org/10.1596/41533.
5) WHO. (2015). Global Action Plan on Antimicrobial Resistance.
6) European Commission. (2017). A European One Health Action Plan against Antimicrobial Resistance (AMR).
7) Le et al. (2020). Repurposing human kinase inhibitors to create an antibiotic active against drug-resistant Staphylococcus aureus, persisters and biofilms. Nature Chemistry 12(2):145-158.
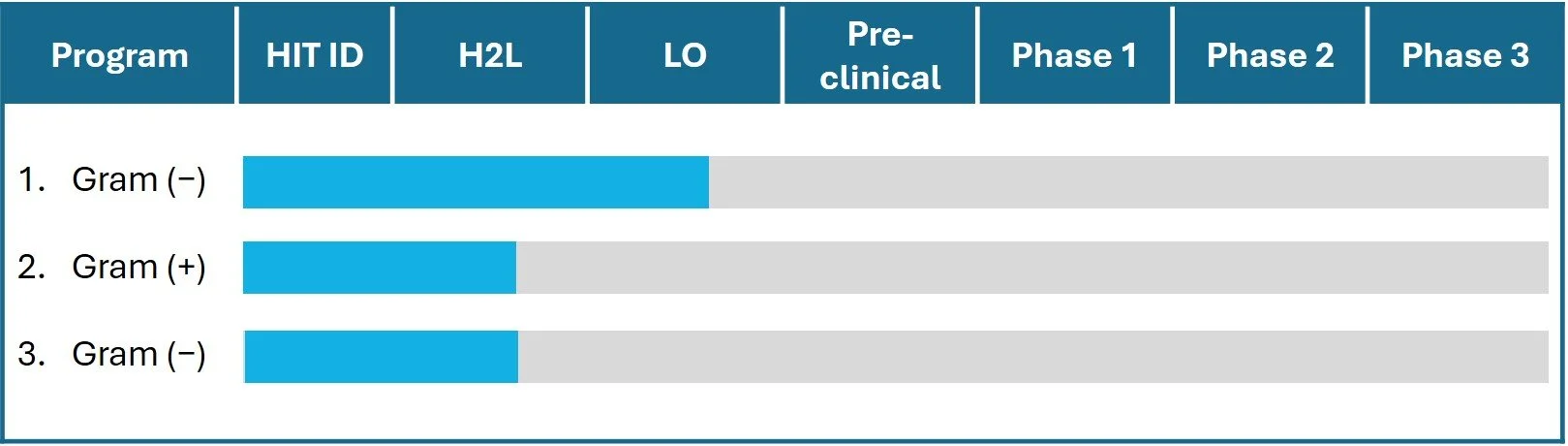
Our pipeline
The smartbax pipeline is centered around highly regulated hydrolase targets.